Sexually Transmitted Infections




Changes in Terminologies:
Venereal Diseases (1500AD-1974) Five Classic Agents
Five classic agents were once thought to be due to sexual indulgence (venery). The sufferers were treated with moral conviction instead of compassion. Death, deformity, and chronicity of the disease process were imminent to the patients who also became victims of social prejudices. The discovery and use of penicillin in the 1940s revolutionized the chronicity. The clinical outcome became shorter. The subject of venereal disease was also put aside by the medical profession.
Sexually Transmitted Diseases (1974-1988) More Than Twenty Causative Agents Added
The term adopted by the World Health Organization (WHO) to describe how the disease is spread with the intention to change the old view of social embarrassment and moral stigma associated with sexual intercourse. More than 20 different causative agents were added to the first classic venereal diseases. The misuse of antibiotics also causes superinfections (total resistance to penicillin) in particular gonorrhea (supergonorrhea) causing recurring symptoms and eventually cases became silent. Acquired immune deficiency syndrome (AIDS) in the early 1980s renewed medical interest.
Sexually Transmitted Infections (1994-to date) Silent Infections
The term was renamed by the WHO because majority of these infections remained silent for many years. The delayed manifestations lead to the recognition of other syndromes like Reiter’s (arthritis, conjunctivitis, discharge), infertility, previously with idiopathic etiologies. Causes for prostate diseases today is being reviewed and STI is being reconsidered as a possible etiology. Recently, in 2019, the first case report of sexually-acquired dengue fever was reported in Spain.
Definition
Generally, they can be defined as infections usually acquired during sexual intercourse. In some cases, transfer is through non-sexual i.e. pregnancy, infected needles and through direct contact with contaminated materials (toilet seats, towels). If not treated, the quality of life may be severely affected not only to the few individuals but also to the global community.
Silent Epidemic
The asymptomatic nature (suppressed incubation) allowed this group of infections to contribute to the growing numbers of undetected cases; thus, has become a silent epidemic.
Causative Agents and common presentations (Table 1)
These causative agents can be categorized into 4 main groups based on their structure, function and treatment.
Generally, the clinical presentations may also be classified based on where they will manifest.(Localizes, generalized and a presentation of reproductive in nature).
Table 1
Causative Agents and Common Presentation of STIs
| CAUSATIVE AGENTS |
PRESENTATION | |||
| DISCHARGE | DERMATOLOGIC | SYSTEMIC | Pediatric | |
| Bacterial | Gonorrhea | Syphilis | Chlamydia | Neonatal Jaundice |
| Fungal | Candidiasis | Tinea Cruris | Pneumonia | Thrush |
| Parasitic/Protozoan | Trichomoniasis | Pubic lice | Toxoplasmosis | Premature delivery and Low birth weight |
| Viral | Herpes Simplex Virus (HSV) | Human Papilloma Virus (HPV) | HIV and Dengue Virus | Mental retardation and Deafness |
BACTERIAL
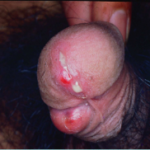 Gonorrhea (Excess flow of seminal Fluid)
Gonorrhea (Excess flow of seminal Fluid)
Purulent discharge (note on picture), from affected area usually manifested within seven days from exposure. Untreated, may cause recurrent urinary and reproductive tract disorders.
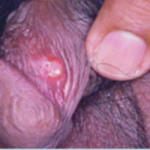 Syphilis
Syphilis
Presents in three stages. In the first stage (within 90 days), a small solitary sore (picture) will appear in the affected area and will disappear within three weeks without treatment. Second stage appears a year later as a generalized rash including the palms and soles (syphilides). Third stage causes body deformity and brain tumors. It can also be transmitted to the newborn and cause deformities.
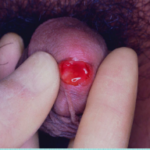 Chlamydia
Chlamydia
Originally responsible for an epidemic of eye disease causing blindness in newborns in the early 1900s (trachoma). It commonly causes a scanty mucoid discharge in affected areas (picture). It may be responsible for reactive arthritis (autoimmune response).
 Beta-Hemolytic Strep
Beta-Hemolytic Strep
Intestinal and vaginal bacteria found in asymptomatic pregnant women. Can be passed on during sexual intercourse. Causes neonatal sepsis and jaundice.
FUNGAL
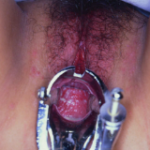 Candidiasis
Candidiasis
Common chronic recurring vaginal disease (picture) in women, who are taking oral contraceptives and antibiotics. Pregnancy and chronic illness like diabetes is also a risk factor for its recurrence. Moisture due to use of nylon underwear and tight-fitting pants are contributory for its recurrence. The condition can be passed on even in monogamous intimacy.
 Tinea Cruris
Tinea Cruris
Fungal infection affecting the skin of the genitals due to excessive moisture. Can cause ping pong infections among monogamous couples.
 Pneumonia
Pneumonia
Fungal pneumonia is a common occurrence with individuals with active HIV infections. It also occurs in individuals with long term exposure to antibiotic treatment.
 Thrush
Thrush
Common in newborn and can be acquired during vaginal delivery.
PARASITIC/PROTOZOAN
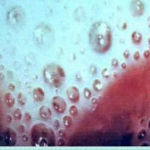 Trichomoniasis
Trichomoniasis
Causes a frothy discharge with an unpleasant smell from affected areas. It can result to premature delivery and low birth weight to neonates.
 Pubic Lice
Pubic Lice
Infestation with crab lice of pubic hair. It causes severe itchiness of the pubic area and red specks on the underwear.
 Toxoplasmosis
Toxoplasmosis
Brought about by ingestion of contaminated food from fecal materials of infected cats. Pneumonia may develop in individuals infected with HIV.
VIRAL
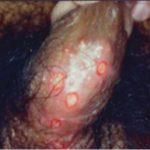 Herpes Simplex Virus (HSV)
Herpes Simplex Virus (HSV)
Generally, infection occurs after around ten days of exposure, small multiple blisters (picture) will appear, breaks and turn into shallow erosions. Heals without treatment within ten days (self-limiting) and while it recurs like the common cold, there are no serious consequences in most cases.
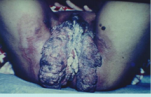 Human Papilloma Virus (HPV)
Human Papilloma Virus (HPV)
There are many types, where all cause small warty growths around the affected areas. Once removed, the recurrence is rare. Types 16 and 18 are linked to cervical cancer, but once diagnosed early, the treatment has a high success rate.
 Human Immune deficiency Virus (HIV)
Human Immune deficiency Virus (HIV)
HIV prevents the immune system from protecting the body from all infectious agents thus the term AIDS. Common presentations are persistent fever of more than two months, recurring pneumonia, diarrhea, and skin cancers. The average incubation period is fifteen years.

Cytomegalovirus Infection (CMV)
CMV is the cousin of HSV. This infection is more widespread. It can be passed on during childbirth and cause mental retardation and deafness.
“Medicine is a Science of Uncertainty and an Art of Probabilities
– Quote by William Osler
GENERALThe approach for diagnosis and treatment taken by most medical practitioners is to utilize guidelines recommended by the American Center for Disease and Control (CDC) or from the Word Health Organization (WHO). Syndromic approach is the most utilized diagnostic and treatment tool for STI patients. This approach however uses only signs and symptoms coming from patients without the benefit of an objective professional evaluation and examination from physicians.
The Syndromic approach Is a subjective assessment and is responsible to the conversion of STI patients to Silent Carriers. These carriers also end up with a false sense of security that they are well only to end up with a poor quality reproductive future.
The Manila Protocol utilize objective parameters taken from the use of reliable patient profile, medical history, physical examination and the use of sensitive and specific diagnostic workup. This minimizes the risk of recurrence due to poor contact tracing and insufficient treatment. The results are higher success rates, better quality of reproductive future which everyone deserves.
Patient Profile
Determining age, gender, coitarche, marital status, patient reliability (to mention a few)These information help assess reliability of information, and risk factors. All of which are predictors of developing a particular disease.
Medical History
Make use of grading system such as symptom score, visible signs, symptoms associated when it was first noticed in line with the time frame of exposure/s. This helps in establishing incubation periods, clinical course important in determining the most likely disease agent.
Physical Examination
This involves a visual and protected examination of lesions the patient may have. The added information adds more depth and adds objectivity to the above subjective data. At this point of the evaluation the physician will have both subjective and objective data making the medical puzzle give a clearer picture.
Diagnostic Aids
Laboratory and other ancillary examinations are only aids for documenting the stage and gauge the severity of the diagnosis. These aids are only helpful in monitoring the progress of a disease in respond to treatment. There are 2 types of diagnostic aids, a screening and specific examinations. Screening examination are useful exams to determine when to do and what specific examinations can be done.
Screening Examinations
Microscopic Examinations
Generally useful for screening, easy to perform, results are readily available for a quick decision making. It is useful in monitoring patient respond to treatment. Example of which is the use of wet mount to count WBC. It can be use to screen the presence of microorganism and differentiate them from each other, example would be grams and giemsa stains. Use of microscopic filters such as dark field examination can visualize the organism causing syphilis and fungus.
Antigen-Body Testing
These are useful as a screening tool for suspected infectious agents. Results are faster as compared to confirmatory test. The downside for this procedure are the false negatives and false positives, consequently under and over treatment cannot be avoided. Examples are ELISA, Immunofluresence, Particle Agglutination Test. All of which can have cross reactions giving false positives. They are also dependent on the stage of the disease. Taken too early will yield false negatives.
Specific Examinations
Cultures and Sensitivity
This laboratory examination grows the suspected bacteria using nutrients that will favor its growth. Sensitivity test will determine which antibiotic will eradicate the isolated pathogen.
Molecular Biology
This test is very specific. A positive test cannot be denied as false. It uses DNA technology. False positives can still occur if taken during resolution of the disease and can consequently lead to over treatment. False negatives will also occur if taken too early in the clinical course and if the specimen is not taken properly hence undertreatment will be a consequence.
Summary for Diagnosis
Medical history and physical examinations are mainstays for reasonable diagnosis. Ancillary examinations should never be taken without responsible extraction of clinical data.
Treatment requires the use of specific antimicrobials taken at the correct dose, intervals, whether the mediations are taken on an empty stomach or not. There are medications that are not absorbed into the body with food and therefore will be useless.
Only Gonorrhea is eliminated within 12 hours with a high dose (pulse dose), single dose antimicrobial given Intramuscularly or orally. The same medication should never be given twice. Serial dosage are useless and harmful. Chlamydia on the other can respond to another class of antimicrobial given single dose however elimination of the infection may take 10 days. A more effective medication is given on a twice a day, minimum of 14 days maximum of 30 days and an average of 21 days. The latter has a higher success rate compared to the single dose. The downside is patient compliance. Gardenella Vaginalis and Trichomoniasis both respond with high success rate to medication also given single dose.
Recurrence mostly are due to reinfection, poor patient compliance, and medications not taken correctly. Fungal infection occurs and can be mistaken for treatment failure when in fact antibiotic intake predisposes to fungal infection.
Objective verification of cure is a must. Presumptive cure leads to the development of silent carriers, resistant strains, and certainly a poor reproductive future.
Viral infections like herpes are self-limiting and, in most cases, they are best managed by patient education and wound care. There is no objective evidence that viral vaccine prevents cancer as a matter of fact it gives a false sense of security, thus the gold standard of a yearly cervical colposcopy is omitted. Cryosurgery has an impressive success rate for cancer in situ.